
Table of Contents
Last Updated on
These two treatments are synonymous with hypothyroidism.
They are the most popular and often prescribed hormone replacements for those suffering from an underactive thyroid gland.
Ostensibly, Armour Thyroid and Synthroid are similar drugs. Their purposes are both the same—provide more thyroid hormone that your body desperately needs.
They also have similarities as well—patients who take either drug, usually end up taking it for the rest of their lives.
However, what differentiates these medicines, are the methods in which these drugs accomplish this.
A layman’s definition would be that Armour Thyroid is natural while Synthroid, similar to its name, is synthetic. Indeed, their differences seem deceptively simple, while being gracefully massive.
This article provides a thorough overview of Armour Thyroid and Synthroid, starting at the point in history when they were first discovered and commercialized, to their current uses today.
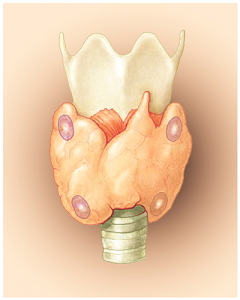 Armour Thyroid
Armour Thyroid
The original thyroid treatment, Armour Thyroid has been relieving the symptoms of hypothyroidism for over a century through animal extract hormone replacement therapy.
Armour Thyroid contains two thyroid hormones, thyroxine (T4) and triiodothyronine (T3), that are extracted from the thyroid glands of pigs.
However, since animal extracts are used, there are excessive amounts of T3 relative to T4 when compared to normal human hormone levels. Depending on your thyroid levels, this may be important information when deciding which treatment to pursue.
Studies have also shown the effectiveness of Armour Thyroid decreasing the size of goiters and treating thyroid cancer. The price for 30 tablets of 60mg of Armour Thyroid is around $25.
Because this drug contains pig thyroid glands, it is not popular with vegetarians, Muslims, and those allergic to pork products among others.
History

George Redmayne Murray (1865-1939)
The origins of using animal extracts are quite old. In 1891, George Redmayne Murray, a pioneer of endocrine disorders, introduced the first thyroid preparation in the world.
One of his patients, a women of 39 years, was suffering from a case of Myxedema, also known severe hypothyroidism. Murray decided to use a novel method in an effort to treat this life-threatening illness.
He extracted the thyroid of a sheep, pounded it into a powder, and injected it into the patient.
Although the effect was not immediate, the symptoms of Myxedema soon began to disappear in the patient. Murray was successful. The patient continued treatment up until she died at 91, a total of 52 years.
Murray’s method and findings, published in Annals of Internal Medicine, spurred the use of animal extracts to treat hypothyroidism particularly in North America, but also throughout the world.
Of course, improvements were made as the years passed. Injections of thyroid glands were often costly, required doctor assistance to take them, and presented the issue of some thyroid hormones being rejected.
Instead, manufacturers created pills of desiccated thyroid extracts by grounding the thyroid gland into a powder, applying binding chemicals (helps absorb the hormones better), and then pressing this combination into a pill.
Doctors also determined that desiccated thyroid extracts from pigs were more effective than other animals such as sheep and cattle.
As more doctors and patients discovered this thyroid treatment, the demand rose as well. Many companies attempted to create treatments using thyroid glands in response to the new market. A lot of these companies failed.
However, the most well-known and effective of these was Armour and Company, the largest American meatpacker and owner of slaughterhouses in the 1900s.
Since Armour and Company had access to all the offal, or organs, of the animals through their already established business, they were able to dominate the thyroid treatment industry easily. The Armour brand later split up, but the name still stuck to the thyroid treatment we know today.
Use Today
 Although not as popular as levothyroxine, Armour Thyroid, and similar drugs such as Westhroid and Nature-Throid, are still used today.
Although not as popular as levothyroxine, Armour Thyroid, and similar drugs such as Westhroid and Nature-Throid, are still used today.
Some patients prefer the idea that this drug is all-natural since it is made from the thyroid glands of pigs. Others like it because it contains a combination of T4 and T3 hormones. Most doctors, however, tend to avoid Armour Thyroid and similar thyroid extracts.
Most do not like that there seems to be a high level of variation in hormones. For example, even though the tablet will state 60 mg of desiccated thyroid, the actual thyroid hormones can be anywhere from 20 mcg to 50 mcg. The intense marketing campaign by levothyroxine manufacturers (later discussed in detail in the Synthroid ‘Use Today’ section) certainly did not help either.
Regardless of the reasons, Armour Thyroid was dropped from most medical curriculums about 50 years ago. It is not uncommon today for doctors to have not heard of desiccated thyroids being used to treat hypothyroidism.
It is certainly an old medicine. However, that does not mean that it is outdated. Some patients who have tried both treatments, religiously prefer Armour Thyroid.
Cautions and Side Effects
If your doctor prescribes you Armour Thyroid, he/she believes that effects of this drug will help you and outweigh any potential side effects. However, it is still prudent to know about the unintended consequences of using Armour Thyroid.
The most common side effect of Armour Thyroid is hair loss. For most, this is temporary and occurs only during the first three months when your body is still adjusting to the treatment. However, some patients have experienced continued hair loss after this period.
The rarer side effects are: headaches, fatigue, changes in appetite and weight, and rashes. Forest Laboratories recommends you stop using Armour Thyroid and see a doctor immediately if you experience allergic reactions such as severe dizziness, trouble breathing, or chest pains when taking Armour Thyroid.
These two side effects that are very, very rare but are life threatening. Studies have also shown Armour Thyroid interacts with birth control pills, blood thinners, insulin, and thioamides, decreasing the effectiveness of all these drugs. Make sure your doctor knows all the other drugs you might be taking before using Armour Thyroid and similar drugs.
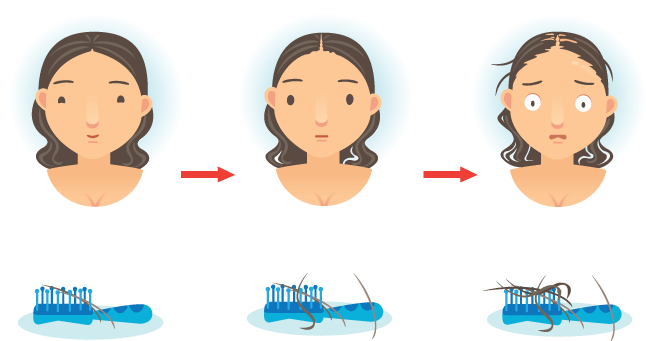
The Most Common Side Effect
It is important to mentally, or even physically, record the dates and times that you take Armour Thyroid.
The reason for this is that it is easy to overdose on this drug. It is quite dangerous as well. If you take more Armour Thyroid than your doctor recommends, you will end up having too much thyroid hormones, a condition known as hyperthyroidism. With this comes unpleasant feelings of anxiety, irritability, confusion and fevers.
If a patient takes too much thyroid hormone they will even develop irregular heartbeats and palpitations, the feeling when you heart skips a beat. For this reason, Armour Thyroid recommends that if a patient misses a dose, they take one right away, but skip the next scheduled one.
In essence, don’t take extra medicine to make up for the missed dose. This might be a problem with those who are already forgetful and don’t have the best memory.
 Synthroid
Synthroid
For over 50 years, Synthroid has been the most popular treatment for people with hypothyroidism, including the most severe cases and is the most commonly prescribed medication in the United States.
It’s purpose is to replace the thyroid hormones produced in the body. However, unlike animal extracts that contain T3 and T4 hormones, Synthroid contains only T4.
Some doctors prefer this as it allows patient’s thyroid glands to control the production of the active hormone, T3.
Numerous studies have supported the claim that Synthroid reduces hypothyroidism symptoms and treats thyroid cancer.
However, there are also others who believe that Synthroid and other levothyroxine drugs cause TSH suppression. These doctors often combine Synthroid with another drug that contains T3.
This isn’t just an intuition, however. Studies have also noted that genetic mutations in 12% to 36% of the population results in bodies converting lower amounts of T4 to T3.
For this group of the population, only levothyroxine treatment may not be enough to relieve the symptoms of hypothyroidism.
Synthroid is available in over 10 different dosages ranging from 25 micrograms to 300 micrograms. Doctors recommend taking Synthroid in the morning on an empty stomach since some foods and other pills can hamper the absorb of the hormones in this drug.
History

Edward Calvin Kendall (1886-1972)
23 years after George Murray successfully treated his myxedema patient, in 1914 American chemist and Nobel Lauerate Edward Calvin Kendall discovered and isolated 7g of thyroxine, what we now call T4, from 6500 pounds of thyroid glands extracted from hogs.
When some hypothyroid patients were treated with Kendall’s thyroxine, it was discovered that this medication was very active in relieving the symptoms of low thyroid hormone.
Three years later, Kendall published a structure he thought to be thyroxine and synthesized it the same year in 1917.
However, ten years later, it was discovered that Kendall was incorrect regarding the structure of thyroxine.
In three papers published during 1926 and 1927, biochemists Charles Robert Harington and George Barger improved upon the process of isolating thyroxine, refuted Kendall’s thyroxine structure, determined the correct structure, and synthesized the first actual thyroxine hormones.
Yet, Harington’s work was not finished. Thyroxine occurs in our bodies as a mixture of the levo and dextro forms of the hormone. Harington recognized that the amino acid stereoisomer (levo) of thyroxine produces much more activity in the thyroid rather than the sugar form (dextro).
Finally, in 1949, after several more advances in the mass extraction of Thyroxine, Glaxo Laboratories, now known as GlaxoSmithKline, launched the first commercial product of levothyroxine.
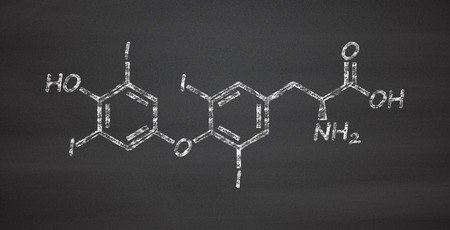
The structure of Thyroxine (T4) discovered by Charles Harington.
However, it was not until Knoll Pharmaceuticals in New Jersey produced the brand-name Synthroid, in 1955, that it became the popular drug we know today.
Marketed as being superior to animal glandular extracts, many doctors and patients sprung to be at the forefront of medical history. It certainly didn’t help that Armour Thyroid during this period also underwent a scandal of sorts where the drug was found to have potency problems, unreliable preparation, and inadequate quality control.
Popularity of animal glandular extracts, like Armour Thyroid that dominated the market for over 40 years, started its decline—a slope that continues today.
Use Today
The popularity of levothyroxine is due to an intense marketing campaign similar to the internet, TV, and radio ads you see for prescription drugs today.
However, of course the internet wasn’t even invented back then and TV was very limited. The manufacturers of levothyroxine, such as Synthroid, decided to focus their efforts on convincing doctors and schools on the benefits of levothyroxine compared to Thyroid drugs created from pig glands.
Would you rather have a drug made from the insides of an animal that spends all day in the mud, or that of one made in a clean, high tech laboratory? The idea almost sells itself, and it is easy to see why many would prefer prescribing to Synthroid than Armour Thyroid.
Synthroid further strengthen its hold on the market by making large contributions to medical schools.
These schools then changed their curriculum to the idea that only the thyroxine hormone needs to be replaced in treatment and recommended their doctors prescribe levothyroxine.
It has stayed that way ever since then. It didn’t help the makers of Armour Thyroid that their drug was having problems during this period. As mentioned before, it is not uncommon for doctors to have not heard of Armour Thyroid because it is no longer being taught in schools.
Levothyroxine has been the most commonly prescribed drug in the United States for the last three years.
Over 120 million prescriptions are filled each year. The most common method of delivery is an oral tablet, but injections and infusions are available as well.
It’s no surprise that levothyroxine accounts for 99.7% of all thyroid hormone replacement drugs. According to a study published in 2009, Armour Thyroid holds only 0.008%.
Cautions and Side Effects
As with Armour Thyroid and other prescription drugs, your doctor believes that the effects of this drug will help you and outweigh any potential side effects. However, it is still prudent to know about the unintended consequences of using Synthroid.
 Most patients experience the benefits of Synthroid after a week of treatment.
Most patients experience the benefits of Synthroid after a week of treatment.
Patients with hypothyroidism feel a lot better, as if they were lifted from a cloud of fog.
However, this is also the period where the side effects start to appear for some. Although levothyroxine is identical to the thyroxine the body produces, added chemicals for absorption lead to unwanted and irritating consequences.
It is also interesting to see that some studies have suggested that prolonged use of Synthroid contributes to lower bone mineral density at the hip and spine areas.
Hair loss is one of the primary side effects, although it is not as common in Synthroid when compared to Armour Thyroid.
Other prevalent ones include: increased sweating, mood swings, and headaches.
Allergic reactions to Synthroid are very rare, but can be life threatening. The makers of Synthroid recommend seeking immediate medical help if you get severe dizziness, trouble breathing, or chest pains.
Overdosing on thyroid hormones is another problem that is often present. If too much thyroid hormone is ingested, it drastically increases the risk for abnormal heart rhythms, heart failure, and heart attacks.
This risk is amplified even further if the patient already has an underlying heart problem.
As with Armour Thyroid and other prescription drugs, make sure patients take their dose at a regularly scheduled time every day. If you miss a dose, the makers of Synthroid recommend you take one as soon as possible, but skip the next dose.
As with all prescriptions, Synthroid can also affect the interactions of other drugs. The effects of blood thinners, for example, jump straight up. This leads to a much higher chance for bleeding all through the body and sudden bruises. Always be sure your doctor knows which drugs you are taking so informed decisions can be made.
Wrapping It Up
 We explored the history, origins, uses, and side effects of two of the most popular hypothyroidism medications, Armour Thyroid and Synthroid.
We explored the history, origins, uses, and side effects of two of the most popular hypothyroidism medications, Armour Thyroid and Synthroid.
Many websites may claim that one drug is the best, and it will completely reverse the symptoms of hypothyroidism.
We’ve all seen hundreds of websites that claim natural thyroid hormone extracts are better for you. And then we’ve seen another hundred that say otherwise. But the truth is there is no single ‘best’ treatment for an underactive thyroid.
Each patient reacts differently to drugs. You may be one of the lucky few that love their thyroid treatment and never change from it. Maybe thyroid supplements work best for you. There are also other ways of improving thyroid levels naturally.
However, it is not unlikely patients will end up trying several thyroid treatments, before settling on one.
Knowing the history and current uses of these medications can help patients and others make informed decisions that raise thyroid hormone levels and better their health, as well as those around them.

I hate Synthroid-it made me a vegetable-no memory-no life- I HATE IT_IT also made me psychotic on certain doses——-so glad to have Armour.. SOOOO glad- just wish other doctors would recommend it more. I will not move from the state of Illinois because they will give Armour-other states not so much so – hate that doctors are dumb on situations like this.
Hi Dana,
Thanks for letting us know. I’m glad you found the medication that works best for you!
My doctor has me taking both Armour and Levothyroxine at the same time. Is that dangerous?
My T4 was low and T3 was good on Armour. My doctor prescribed 25mg of Levothyroxine. Just started today with both. Will see what happens.
I’ve been on both levothyroxine & armour thyro. Difference for me: levothyroxine =being a slug, not able to do anything but sleep or Armour=be my normal self doing all my house cleaning & working 40-50 hr a week. BIG DIFFERENCE:)
The generic may help. NP THYRO. My insurance will not cover the Armour. But I was told that if the Dr writes a letter stating that you require this. Example: allergic to the ingredients in the medication. They will allow it.
Back in the day I was put on Synthyroid. I was in my late 20’s and so uninformed. I felt better for 10 minutes (literally) and felt I was listening to my body, if you know what I mean. So I asked my pharmacist if Syn of Synthyroid meant synthetic thyroid. He said yes. I asked “is there was a natural thyroid med?” He said yes and I was put on Armour from a very disgruntled doctor. But now a days you have to fight tooth and nail to get Armour and only if you find an old doctor that will prescribe it. This can happen when you move to another location. I was driving from Oregon to back to my doctor in No. California to get my Armour Thyroid prescription. The visit in California cost $58.00, the lab just $92 and he prescribes Armour. Here in Oregon they have a “Rule of 4” I do believe and in my opinion, I think Medicare should investigate. You have to see a doctor 4 times $350.00/visit and the lab is $250-350. And they won’t prescribe Armour. The trip to California more than paid for itself. But want to mention here that my doctor in California has a personal oath and ethic to not take “commission checks, trips and/or bonus” from the pharmaceutical companies as an inducement to switch to not so natural Nature or Syn Thyroid brands.
Why would I want to take a chemical thryroid replacement? What happens to my thyroid while a chemical is doing a lousy job replacing it. And why wouldn’t I want a natural thyroid med that works with my somewhat heathly thyroid. My body knows the answer. Armour is my body’s thyroid replacement of choice and I’ll go with my body.
Is it safe to take levothyroxine in the morning and armour in the evening?
I have spent many years on synthroid with many side affects and my thyroid levels always see sawed. It was only until I started on Armour thyroid that my thyroid finally showed signs of stabilization. I have gone from 120 mg Armour to 90 mg and now my thyroid levels are within range. And, I have noticed since my thyroid levels have stabilized, my blood pressure has too. I suffered from high blood pressure for years, and after extensive research I discovered that if you suffer from thyroid issues you are more than likely have blood pressure issues.too. Blue cross pays for my armour thyroid and my cost is just a couple of dollars for a 60 day supply. I swear by Armour thyroid. By the way my great results are due to switching from a traditional doctor to a holistic one.The difference has been amazing.
I have a Medicare precription drug plan through Blue Cross/Blue Shield and Armour Thyroid and it usually costs me about $44 for a three month’s supply (90 tablets). I get it shipped free through Express Scripts.
Thank you for the information. Now that I am on Medicare, Armour Thyroid is not covered by any insurance. Prior to reaching the “Medicare nightmare” my Armour Thyroid was always covered, costing me $4, as opposed to the current out-of-pocket $196. I need a way to plead my case to the insurance companies, so your information is helpful. Many years ago a doctor prescribed Synthroid for me. All I did was stare at a wall. Needless to say, that was a disaster for my academic work. Thanks.