Table of Contents
Last Updated on
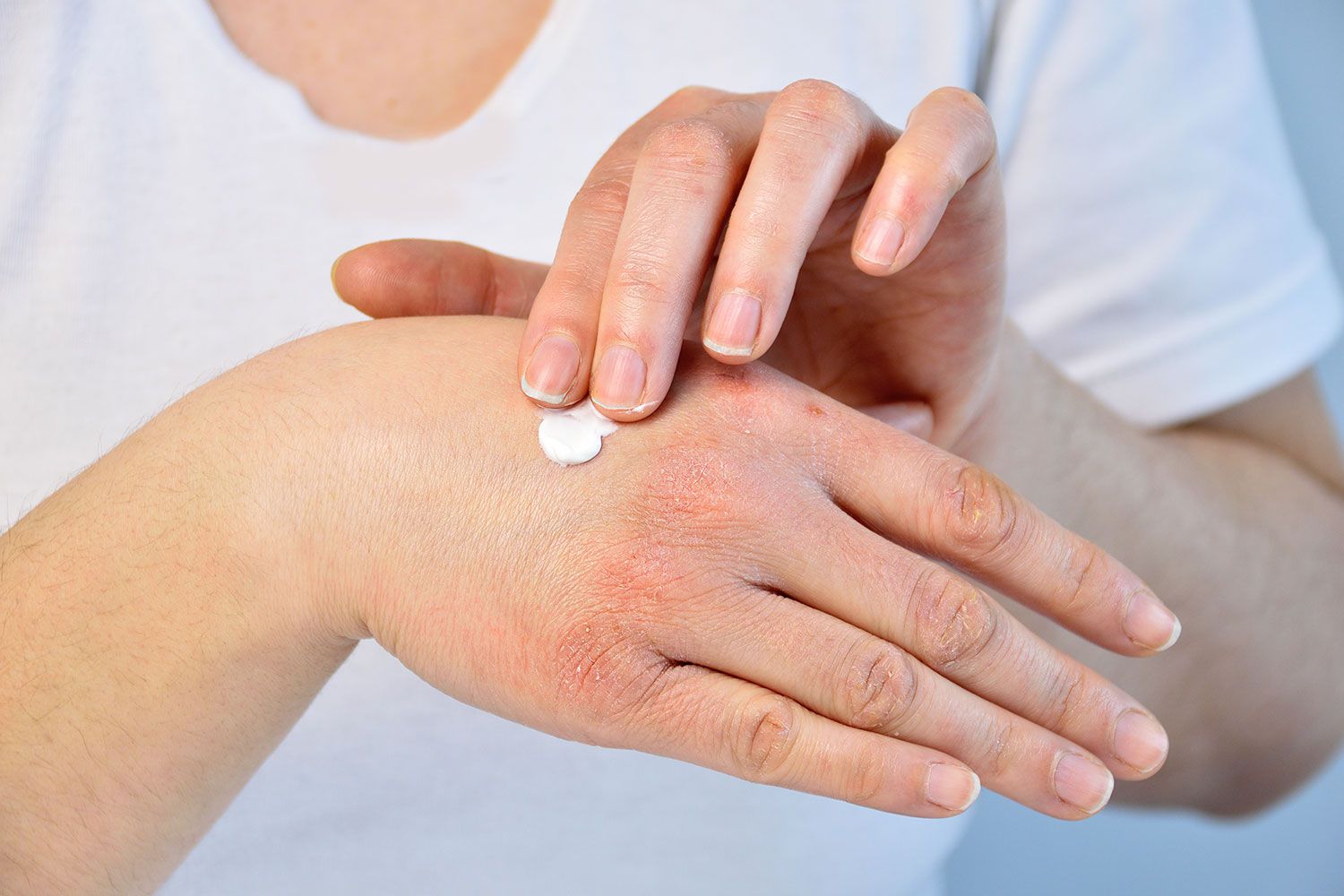
Could Thyroid Problems Cause Skin Rashes?
There are many symptoms to be expected when it comes to the different thyroid problems, given how important and involved the thyroid is with body functions.
But are skin rashes expected to develop as well? Can skin rashes be used to detect the underlying presence of a thyroid problem of some kind?
What are the most common thyroid problems?
The thyroid gland is a very important body organ. Through the production and secretion of the two thyroid hormones – thyroxine (T4) and triiodothyronine (T3), it is responsible for multiple body functions.
Unfortunately, the thyroid gland is often affected by hypothyroidism or hyperthyroidism – the two most common thyroid problems.[i]
As a result of the low production of the thyroid hormones, a condition known as hypothyroidism develops. It characterizes itself with symptoms such as cold intolerance, fatigue, weight gain, depression, constipation, muscle, and joint aches, etc. [ii]
On the other hand, as a result of too much thyroid hormones being produced, a condition known as hyperthyroidism develops. Some of the most characteristic hyperthyroidism symptoms include an enlarged thyroid gland, hyperactivity, diarrhea, mood changes, sensitivity to heat, etc. [iii]
Different skin rashes as symptoms of thyroid problems
Since thyroid hormones take part in regulating so many different body functions, it is expected that various different symptoms develop if the normal thyroid levels are off.
It should not come as a surprise to find out that thyroid problems affect our skin as well.
In fact, there are several different skin rashes that develop as a symptom of the most common thyroid problems.
Based on the skin rash, a dermatologist can help in diagnosing the underlying cause.
In the following article, we will cover the most common skin rashes that develop as a symptom of thyroid problems.
Dry Skin
We all have had our experience with dry skin, and for some of us, dry skin might be the sign that our body is using to let us know about the presence of hypothyroidism.
We are talking about a very common skin condition that develops as a result of the lack of water in the epidermis – the most superficial skin layer. [iv]
A number of factors can cause dry skin, and hypothyroidism is one of them. In most cases of hypothyroidism, patients have reported the presence of dry and itchy skin.
In a study published in the Journal of General Internal Medicine, 74% of the participants diagnosed with low-thyroid levels, were discovered to struggle with dry, itchy skin as well. [v]
Like most cells in the human body, the skin cells are regulated by the thyroid gland and its hormones. It is the skin cells turnover rate that is regulated with the help of the thyroid hormones, which is why, once that their production declines, dry skin occurs as a symptom.
Due to the declined production of thyroid hormones, the skin requires a longer time to regenerate, while in the meantime, dry, itchy skin is being formed.
Dry skin, even when linked with hypothyroidism, is usually easily-manageable. Taking your thyroid medications regularly, avoiding any harsh soaps and detergents, and using over-the-counter moisturizers are the usual treatment methods used to treat dry skin. Topical corticosteroids might be used as well, in the more severe cases of dry skin.[vi]
Myxedema
Myxedema is considered to be the classic characteristic skin sign that reveals the presence of either undiagnosed severe hypothyroidism or unsuccessfully treated severe hypothyroidism. [vii]
This is a serious condition that requires treatment right away, as severe hypothyroidism may have caused it to begin with.
The most noticeable symptoms of myxedema are the swelling of the face, which can spread to your lips, eyelids, and even your tongue, but also swelling and thickening of the skin anywhere on the body.
Myxedema is most characteristically affecting the skin on the face and the legs – especially the lower legs. Because myxedema can cause a variety of complications, if left untreated, including heart failure, pregnancy issues, hypothermia, kidney problems, and coma, among many others, it is of vital importance to be treated right away.
The usual treatment for myxedema is taking a proper amount of the synthetic version of thyroxine to restore the body’s levels of this important hormone. Taking your medication regularly is essential to prevent any new development of the symptoms of myxedema. By doing so, you will be able to prevent myxedema from developing ever again and control all of your other hypothyroidism symptoms efficiently as well.
Acne
You might have thought that you have left those days behind you, and yet, the acne is still here to cause embarrassment whenever you step away from home.
Adult acne is more common among women compared to men, but it is not the usual hormones to blame, that being progesterone and estrogen for the presence of adult acne. Low levels of thyroid hormones can also cause acne to develop.
Two female reproductive hormones play a very important role in acne prevention, especially progesterone. But if there is not enough Vitamin A and thyroid hormones in the body, to produce progesterone, acne is expected to develop, as there is a very high risk of that happening.
If you struggle with either Vitamin A or thyroid hormones deficiency, it is almost impossible to avoid acne. [viii]And most doctors, even dermatologists, fail to make the link between acne and hypothyroidism. That is why you might go through several misdiagnosis and unsuccessful treatments before you get your hypothyroidism diagnosed and treated once and for all.
Knowing the roots of the problem, you might think that taking a progesterone supplement might put an end to your suffering. But in reality, that is not the case.
There is no point in taking a progesterone supplement when what your body really needs is a thyroid hormone supplement.
That is why thyroid medication is being used to treat acne that has been caused by low levels of thyroid hormones in the body. Of course, a well-balanced diet and a good skincare routine are also welcomed at this point.
Granuloma annulare
Granuloma annulare is a benign, inflammatory skin condition that is not seen too often. Granuloma annulare causes characteristic red-colored skin bumps to be formed in a certain ring pattern. The skin bumps can become itchy over time. Granuloma annulare affects mostly children and women. There are a few different types of granuloma annulare, of which the localized type is the most common one.
Its causes are yet to be determined; however, it is commonly linked to autoimmune hypothyroidism and thyroiditis, including diabetes mellitus as well.
A study published in the Canadian Family Physician looked at a case of granuloma annulare within a 10-years old female child. After performing some tests, it has been found that the child faced further hypothyroidism symptoms including dry skin, weight gain, and fatigue, and tests revealed low thyroxine levels and high thyroid-stimulating-hormone (TSH) levels.
After levothyroxine has been used, the symptoms, including those of granuloma annulare, were successfully resolved.[ix]
When it comes to granuloma annulare, no specific care is required, but if you want, your doctor can prescribe corticosteroids and recommend ointments. However, if you are dealing with granuloma annulare without being diagnosed with hypothyroidism or any thyroid problem whatsoever, it would be for the best to consult your doctor as soon as possible.
Granuloma annulare, similar as in the case that we have previously discussed, might be the sign that will get your hypothyroidism diagnosed.
Vitiligo
Vitiligo is a skin condition that affects about 1% of the worldwide population. This skin condition causes the melanocytes, which are the skin cells responsible for producing melanin, the skin pigment, to be destroyed.
As a side-effect, areas of the skin where this has happened lose their color and turn white. The skin areas which are most commonly affected by this condition are the arms, legs, face, nostrils, genitals, etc.
Vitiligo is considered to be an autoimmune disease, with many possible risk factors to be considered. It has been suggested that patients with other autoimmune diseases have a higher risk of developing vitiligo as well. In fact, vitiligo and alopecia areata are the two most common autoimmune skin conditions linked to autoimmune hypothyroidism. [x]
Vitiligo has been seen in 8% of the patients with autoimmune hypothyroidism, according to a study published in the Indian Journal of Dermatology. [xi]Despite the fact that there is a clear proof of the increased risk of vitiligo in patients with autoimmune hypothyroidism, the link, and the mechanism are yet to be deeply investigated.
The good news is that there are many treatments that you can try for managing vitiligo; however, the bad news is that a cure is yet to be found. Topical corticosteroids have been suggested to restore the skin pigment in some cases. Light therapy to prevent the vitiligo from progressing and spreading might be used as well. There are many other treatments that your dermatologist can recommend to you to manage your vitiligo better.
Conclusion
In conclusion, thyroid problems do cause different skin rashes to develop.
Some skin rashes are more common than others, and some are easier to manage than others.
The important thing to know is that each and every skin problem, especially skin rash, needs to be reported to a professional dermatologist so that he/she can determine if this has been a sign of your body telling you that something is not quite right with your thyroid gland.
References
[i] Nussey, S., & Whitehead, S. A. (2001). Endocrinology: An integrated approach. Oxford, UK: Bios
Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK28/
[ii] Qari, F. (2015). Hypothyroidism in clinical practice. Endocrine Abstracts. doi:10.1530/endoabs.37.ep1007
Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4140009/
[iii] Livolsi, V. A., & Baloch, Z. W. (2018). The Pathology of Hyperthyroidism. Frontiers in Endocrinology,9. doi:10.3389/fendo.2018.00737
Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6286962/
[iv] Pons-Guiraud, A. (2007). Dry skin in dermatology: A complex physiopathology. Journal of the European Academy of Dermatology and Venereology,21(S2), 1-4. doi:10.1111/j.1468-3083.2007.02379.x
Retrieved from https://www.ncbi.nlm.nih.gov/pubmed/17716284
[v] Canaris, G. J., Steiner, J. F., & Ridgway, E. C. (1997). Do traditional symptoms of hypothyroidism correlate with the biochemical disease? Journal of General Internal Medicine,12(9), 544-550. doi:10.1046/j.1525-1497.1997.07109.x
Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1497160/
[vi] Cole, G. W. (n.d.). Dry Skin Causes, Treatment, Remedies & How to Get Rid of It
Retrieved from https://www.medicinenet.com/dry_skin/article.htm#what_is_the_treatment_for_dry_skin
[vii] Safer, J. D. (2011). Thyroid hormone action on the skin. Dermato-Endocrinology,3(3), 211-215. doi:10.4161/derm.17027
Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3219173/
[viii] Adam. (n.d.). Can Thyroid Diseases Cause Acne?
Retrieved from https://www.thyromate.com/blog/can-thyroid-diseases-cause-acne
[ix] Moran J., Lamb L. (1995). Localized granuloma annulare and autoimmune thyroid disease. Are they associated? Canadian Family Physician, 41: 2143–2144
Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2146455/
[x] Baldini, E., Odorisio, T., Sorrenti, S., Catania, A., Tartaglia, F., Carbotta, G., . . . Ulisse, S. (2017). Vitiligo and Autoimmune Thyroid Disorders. Frontiers in Endocrinology,8. doi:10.3389/fendo.2017.00290
Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5663726/
[xi] Puri, N. (2012). A study on cutaneous manifestations of thyroid disease. Indian Journal of Dermatology,57(3), 247. doi:10.4103/0019-5154.96227
Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3371544/

I think I have thyroid problems. I never thought about it until now reading all the info on thyroid and how it affects you. I would like to know more about low thyroid and how can I find out if I have it.