Table of Contents
Last Updated on
When a term hormone comes to mind we immediately think of estrogen, progesterone, and testosterone.
A wide range of hormones are released into our body and all of them have unique functions that are necessary for good health and wellbeing.
Not only do hormones regulate our sexual and reproductive health, but everything else including hunger, food intake, body fat regulation, you name it.
In previous articles, we’ve discussed the impact of progesterone and estrogen on thyroid health, and this post will elucidate the role of leptin.
What is leptin?
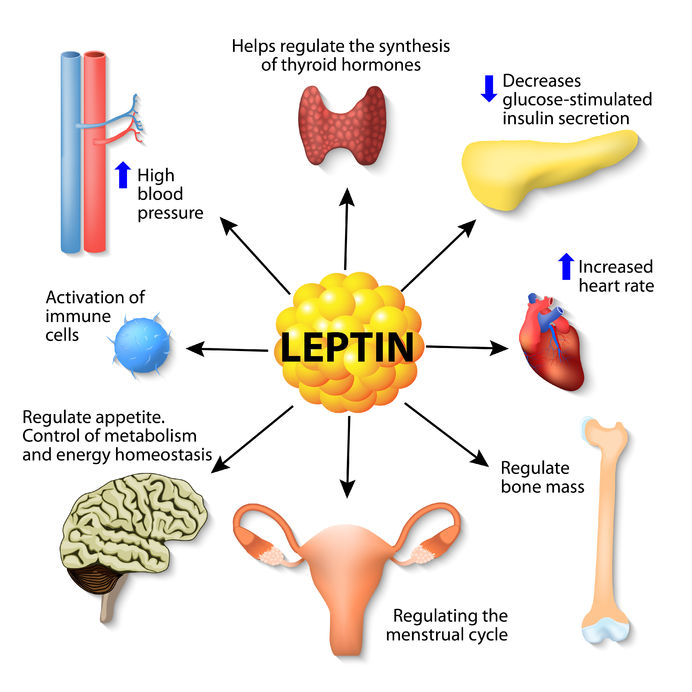
Leptin is a hormone produced by adipocytes or fat cells in the body. The primary role of the hormone is to regulate body fat. Through communication with the brain, leptin controls hunger and behavior and sends a signal to inform your body it’s full and it should stop eating.
Evidence shows this hormone has many other roles such as a “growth factor in various cell types”, a permissive factor for puberty, a signal of metabolic status, a modulation between fetus and maternal metabolism, and it interacts with other hormonal mediators and “regulators of energy status and metabolism such as ghrelin, insulin, the insulin-like growth factors” and others[i].
Leptin acts as both endocrine and paracrine factor, but it can function as an autocrine factor too. To clarify, endocrine signaling is the most prevalent type of cell signaling and it revolves around sending a signal through the body by secreting hormones into the bloodstream.
Paracrine signaling molecules are released from paracrine cells and they diffuse locally through the extracellular fluid, act as mediators by targeting cells nearby[ii].
Autocrine signaling refers to the production and secretion of an extracellular mediator by a cell followed by its binding to receptors on the same cell to kick-start the process of signal transduction[iii].
Leptin, also known as starvation or satiety hormone, targets hypothalamus to regulate long-term energy balance i.e. the amount of calories we eat and expend, and how much we store in our body. The more body fat adipocytes carry, the more leptin they produce.
That’s why this hormone is deeply connected to overweight/obesity and weight loss process.
Leptin’s impact on regulation of thyroid function
Thanks to its role in body fat regulation, leptin takes part in a number of processes in a human body.
One of these processes is regulation of thyroid function.
For example, the dominant signal to the brain that suppresses the expression of TRH (thyrotropin-releasing hormone) in the paraventricular nucleus (PVN) of the hypothalamus is a decline in levels of the hormone leptin.
The TRH controls the release of thyroid-stimulating hormone (TSH) from the pituitary.
Then, TSH acts on receptors in the thyroid to promote synthesis and release of T3 and T4. (see our thyroid feedback loop article)
Decreased concentration of leptin acts through the hypothalamus to reduce energy expenditure, increase appetite, and modify the neuroendocrine function in a direction that puts emphasis on survival.
A drop-in leptin levels involves suppression of reproduction, linear growth, and the thyroid axis parallel to stress axis activation[iv].
Mutation of the leptin receptor gene can be one of the underlying factors that lead to obesity with central hypogonadism and hypothyroidism[v].
In primary hypothyroidism, TRH expression in PVN increases just like production of TSH. However, in a state of starvation TRH expression is suppressed in PVN even though it’s expressed in other areas of the brain. Eventually, production of TSH declines.
The impact of leptin and thyroid function can be both direct via leptin receptors found in TRH neurons and indirect through different pathways including melanocortin pathway. Melanocortin system is involved in body weight regulation through its role in appetite and energy expenditure via ghrelin, leptin, and other hormones.
The Journal of Clinical Investigation published a study which found that hypothalamic melanocortins can stimulate thyroid axis and their antagonist known as Agrp (agouti-related peptide) can inhibit it.
Administration of the Agrp antagonist decreased TSH levels and led to a long-lasting suppression of T4 thyroid hormone.
The study also showed that leptin increased TRH release and confirmed that melanocortin system plays a big role in the fasting-induced suppression of hypothalamic-pituitary-thyroid axis[vi].
Leptin and thermogenesis
Thermogenesis, coming from the Greek word thermos for heat, is a metabolic process during which the body burns calories to produce heat. The process of thermogenesis is important for weight management.
For example, people who want to slim down are advised to exercise and eat certain foods to improve thermogenesis and lose more weight.
Several factors contribute to thermogenesis including environmental temperature, starvation, and feeding.
For example, starvation can decrease metabolic rate by as much as 40% while food restriction sufficient to maintain a 10% reduction in body weight is linked to a decrease in energy expenditure.
A paper from the European Journal of Endocrinology explains that feeding heightens energy expenditure through increased metabolic rate by 25-40%.
The report explains that brain detects exposure to cold which leads to activation of efferent pathways whose goal is to control energy dissipation. The primary component of this response is the sympathetic nervous system which innervates thermogenic targets like skeletal muscle and brown adipose tissue.
Experiments wherein hypothyroid rats were exposed to cold revealed that thyroid hormones are involved in the process of thermogenesis at the brown fat level.
While it was a common belief that thyroid hormones had a permissive role in thermogenesis because their levels didn’t change during cold exposure, evidence shows these hormones have been found to rise with increased calorie intake and deplete during starvation.
Of course, this effect is associated with decreasing leptin levels and decreased expression of hypothalamic TRH.
Therefore, scientists explain that declining thyroid hormones contribute to a starvation-induced decrease in thermogenesis and leptin plays a huge role in the process[vii].
Thyroid autoimmunity and leptin resistance
Leptin resistance is characterized by high levels of this hormone, but the brain doesn’t receive the signal and makes you feel hungry. Basically, the brain is starved although the body isn’t. This can lead to overweight and obesity.
A journal Thyroid published an interesting study whose main objective was to evaluate the association between thyroid autoimmunity and obesity.
Scientists wanted to be more specific and decided to analyze whether thyroid autoimmunity and weight gain are connected if hormone leptin was considered the key factor that connected both conditions.
The study showed that leptin resistance could mitigate leptin deficiency and enhance autoimmunity in obese participants. Development of resistance to the weight-lowering effects of leptin might be initiated through inflammatory signaling activation[viii].
In other words, inflammatory component of the autoimmune response contributes to leptin resistance and increase the risk of obesity.
It’s important to mention that obesity is a risk factor for thyroid autoimmunity[ix] too.
Speaking of autoimmunity, a growing body of evidence confirms a link between leptin and inflammation.
Serum leptin levels are elevated in a number of chronic inflammatory conditions including inflammatory bowel disease, pelvic endometriosis, inflammatory nephritis, nonalcoholic hepatitis, Behcet’s disease, chronic pulmonary inflammation, and Graves’ disease.
Graves’ disease is an autoimmune disease that affects thyroid and stimulates overproduction of thyroid hormones. The accepted theory is that increased levels of the hormone leptin in obese persons can contribute to low-grade chronic inflammation.
As a result, autoimmune conditions like Graves’ disease can develop[x] and start attacking healthy cells and tissues.
Interestingly, the American Journal of Physiology published a study which found that leptin could also exhibit an anti-inflammatory role and attenuate systemic inflammation[xi].
Leptin deficiency and thyroid
The function of a butterfly-shaped gland is linked to secretion of leptin by adipose tissue. Leptin deficiency isn’t such a common occurrence, but it alters the circadian rhythm of TSH that leads to central hypothyroidism. Central hypothyroidism is a type of hypothyroidism that occurs due to insufficient stimulation by TSH of an otherwise healthy gland. Unlike other forms of the underactive thyroid gland, central hypothyroidism is relatively rare and affects 1 in 80,000 to 1 in 120,000 people[xii].
The condition has been reported in cases of congenital leptin deficiency, but the exact relationship of leptin deficiency on thyroid hormone production was unclear. A group of scientists from the Australian National University in Canberra carried out an interesting study whose results they published in the journal Thyroid Research.
For the purpose of their research, they included two males aged 5 and 27 and two females aged 35 and 40 prior to and after leptin replacement. The child was followed for four years while adult participants for eight years.
Findings revealed that regardless of leptin replacement, the leptin-deficient participants had a normal thyroid function. Although leptin influences hypothalamic-pituitary-thyroid axis, it’s not required for a normal production of thyroid hormones[xiii], scientists concluded.
Does thyroid influence leptin levels?
Despite the fact that thyroid and leptin are connected, and they are vital for many processes, including weight management, one might think that abnormalities in their function would have consequences of the level of hormones.
The study above showed that impaired levels of leptin don’t necessarily affect hormones produced by the thyroid. At the same time, a research carried out by scientists from Spain revealed that thyroid hormones don’t affect leptin levels.
Sesmilo G. et al found “no correlation between serum leptin and thyroid hormone levels at any time during the study.” Leptin and body fat percentage didn’t change throughout the study in both hypo- and hyperthyroid participants.
Researchers concluded thyroid function isn’t a determinant of leptin levels[xiv].
Hyperthyroidism and leptin
While most studies focus on the relationship between leptin with hypothyroidism and thyroid function in general, some studies also analyzed the relationship between this hormone and hyperthyroidism.
As you’re already aware, hyperthyroidism or overactive thyroid gland is a condition wherein excessive levels of thyroxine are produced. The journal Metabolism featured a study which discovered that serum leptin levels are slightly increased in participants with moderate hyperthyroidism.
The effect was a result of direct action of thyroid hormone. That being said, leptin levels normalized after patients returned to the euthyroid state[xv].
How to normalize leptin levels
Lepin is a vital hormone for many processes in the body including hunger, starvation, thermogenesis, just to name a few. Good health and wellbeing depend on the proper function of both leptin and thyroid.
The quick but also potentially inaugurate way to determine whether you’re leptin resistant is to stand in front of the mirror and check body fat.
If you have a lot of body fat, particularly in the abdominal area, chances are high your body has developed leptin resistance.
Useful ways to normalize levels of this hormone are:
- Fiber-rich diet because fiber regulates digestion and aids weight management. Plus, fiber makes you feel full for longer
- Avoid processed foods
- Get enough sleep
- Exercise regularly
- Consume a protein-rich diet
- Keep cholesterol and triglycerides in a healthy range
Conclusion
Leptin is an important hormone whose role in thyroid function was poorly understood. Both leptin and thyroid are crucial for metabolism, thermogenesis, and other processes occurring in our body.
Studies show that leptin is involved in inflammation and autoimmunity meaning it’s a potential therapeutic target for the management of autoimmune conditions.
References
[i] Margetic S, Gazzola C, Pegg GG, Hill RA. Leptin: a review of its peripheral actions and interactions. International Journal of Obesity and Related Metabolic Disorders 2002 Nov;26(11):1407-33. Doi: 10.1038/sj.ijo.0802142 https://www.ncbi.nlm.nih.gov/pubmed/12439643
[ii] Study guide – cellular communication, University of Kent https://moodle.kent.ac.uk/external/mod/book/view.php?id=2396&chapterid=78
[iii] Autocrine signaling, Science Direct https://www.sciencedirect.com/topics/neuroscience/autocrine-signalling
[iv] Ahmina RS, Prabarkaran D, Mantzoros C, et al. Role of leptin in the neuroendocrine response to fasting. Nature 1996 Jul 18;382(6588):250-2. Doi: 10.1038/382250a0 https://www.ncbi.nlm.nih.gov/pubmed/8717038/
[v] Clement K, Vaisse C, Lahlou N, et al. A mutation in the human leptin receptor gene causes obesity and pituitary dysfunction. Nature 1998 Mar 26;292(6674):398-401. Doi: 10.1038/32911 https://www.ncbi.nlm.nih.gov/pubmed/9537324/
[vi] Kim MS, Small CJ, Stanley SA, et al. The central melanocortin system affects the hypothalamo-pituitary thyroid axis and may mediate the effect of leptin. Journal of Clinical Investigation 2000 Apr;105(7):1005-11. Doi: 10.1172/JCI8857 https://www.ncbi.nlm.nih.gov/pubmed/10749579/
[vii] Zimmermann-Belsing T, Brabant G, Holst JJ, et al. Circulating leptin and thyroid dysfunction. European Journal of Endocrinology 2003;149:257-271 http://www.eje-online.org/content/149/4/257.full.pdf
[viii] Duntas LH, Biondi B. The interconnections between obesity, thyroid function, and autoimmunity: the multifold role of leptin. Thyroid 2013 Jun;23(6):646-53. Doi: 10.1089/thy.2011.0499 https://www.ncbi.nlm.nih.gov/pubmed/22934923
[ix] Sanyal D, Raychaudhuri M. Hypothyroidism and obesity: An intriguing link. Indian Journal of Endocrinology and Metabolism. 2016;20(4):554-557. doi:10.4103/2230-8210.183454. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4911848/
[x] Iikuni N, Lam QLK, Lu L, Matarese G, La Cava A. Leptin and Inflammation. Current immunology reviews. 2008;4(2):70-79. doi:10.2174/157339508784325046. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2829991/
[xi] Flatow EA, Komegae EN, Fonseca MT, et al. Elucidating the role of leptin in systemic inflammation: a study targeting physiological leptin levels in rats and their macrophages. American Journal of Physiology 2017 Nov 1:313(5):572-82. Doi: 10.1152/ajpregu.00171.2017 https://www.ncbi.nlm.nih.gov/pubmed/28768659
[xii] Gupta V, Lee M. Central hypothyroidism. Indian Journal of Endocrinology and Metabolism. 2011;15(Suppl2):S99-S106. doi:10.4103/2230-8210.83337. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3169862/
[xiii] Paz-Filho G, Delibasi T, Erol HK, et al. Congenital leptin deficiency and thyroid function. Thyroid Research 2009 Nov 4:2(1):11. Doi: 10.1186/1756-6614-2-11 https://www.ncbi.nlm.nih.gov/pubmed/19889232
[xiv] Sesmilo G, Casamitijana R, Halperin I, et al. Role of thyroid hormones on serum leptin levels. European Journal of Endocrinology 1998 Oct;139(4):428-30. https://www.ncbi.nlm.nih.gov/pubmed/9820621
[xv] Nakamura T, Nagasaka S, Ishikawa S, et al. Association of hyperthyroidism with serum leptin levels. Metabolism 2000 Oct;49(10):1285-8. https://www.ncbi.nlm.nih.gov/pubmed/11079817
