Table of Contents
Last Updated on
The Possible Connection Between Hypothyroidism And Hypoglycemia: Here’s What You Need To Know
Hypothyroidism is a relatively common condition that can lead to adverse effects on the overall well-being of a patient’s body. This condition is defined as a low level of bioavailable Thyroid hormones in a patient’s body, leading to a reduced metabolism in the body.
This condition can cause a patient to experience a large number of symptoms that can have a significant interference with their day-to-day function. Additionally, the condition can have an adverse effect on certain functions within the patient’s body and, in turn, lead to the development of additional diseases as a complication.
At the same time, however, it is important to note that some diseases and conditions can also cause impairment in Thyroid function. This can then cause Hypothyroidism as a complication.
The connection between Hypothyroidism and Hypoglycemia has recently sparked a lot of attention. The link between these conditions goes both ways. A patient who is diagnosed with an underactive Thyroid may experience complications with their internal regulation of glucose and insulin, which can lead to Hypoglycemia.
On the other hand, a patient who is diagnosed with Hypoglycemia may develop Hypothyroidism as a complication or experience a worsening of their condition and symptoms if they have been diagnosed with autoimmune Hypothyroidism.
Here, we will analyze the connection that exists between Hypothyroidism and Hypoglycemia. We will take a look at the symptoms that may be present in a patient’s body with each of these conditions. We will also consider how each of these conditions can affect the body in such a way that the patient develops the other linked condition.
Finally, we will provide an overview of how the presence of these two conditions simultaneously can be treated more effectively.
An Overview Of Hypothyroidism
Hypothyroidism is one of the most common types of endocrine diseases. This condition may affect as much as 2% of the world’s population and is known to be much more prevalent amongst women when compared to men1.
Hypothyroidism is diagnosed when a patient’s blood contains a low level of Thyroxine, a vital Thyroid hormone that is often referred to only as T4. This is a less potent version of Thyroid hormone but serves an essential purpose as it is converted into the active type of Thyroid hormone, known as triiodothyronine, or T3 for short.
Levels of Thyroid Stimulating Hormone, or TSH, in the patient’s body is often elevated when they suffer from Hypothyroidism, as the Pituitary Gland secretes excess levels of this hormone to stimulate the production of T4 when a low level of this Thyroid hormone is detected2.
Hypothyroidism can cause many symptoms in a patient since all cells in their body depend on Thyroid hormones for its metabolism and overall functionality.
When there is too little of these hormones present in the body, the cellular function starts to slow down. Some symptoms3 to look out for include:
- You may become more sensitive to cold temperatures.
- You may experience fatigue more frequently and feel tired during the day, even if you had a good night’s rest.
- You may start to notice some problems with your cognitive function, such as memory loss.
- You may notice that your skin becomes drier, even when using a moisturizer.
- You may experience depressing thoughts, and if you are already suffering from depression, the condition may gradually become worse.
- You may also start to notice that you frequently experience constipation.
The problem with Hypothyroidism is that the symptoms seem to be different for every patient. The symptoms mentioned above are only a few signs that may signal the presence of a Thyroid dysfunction. Some patients will just experience a single symptom when Thyroid hormone levels in their body become low, while another patient may experience may life-altering symptoms.
This is why obtaining the right type of blood tests is vital to assist with the diagnosis of Hypothyroidism and to proceed with an appropriate treatment plan.
An Overview Of Hypoglycemia
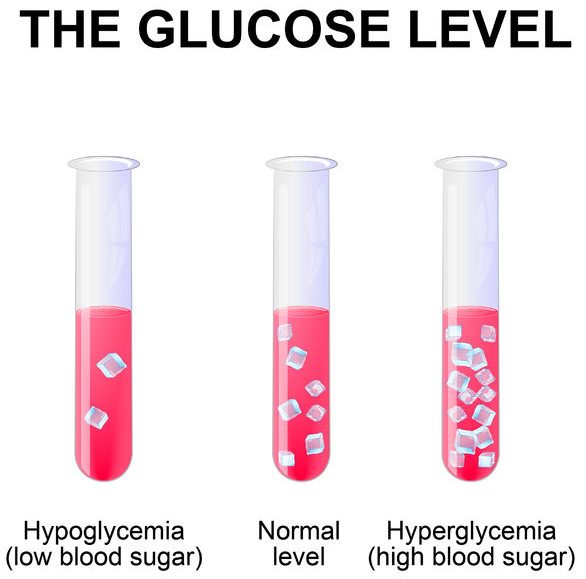
Hypoglycemia is the opposite of high blood glucose levels. When blood glucose levels become very low, then the body can go into shock, and dangerous complications may occur. Generally, a person is considered to be affected by Hypoglycemia whenever their blood glucose levels fall to a level below 4 mmol/L.
The primary symptoms4 linked to a drop in blood glucose levels include fatigue, a dizzy feeling, and sweating.
Other symptoms may also be present in a patient when they experience Hypoglycemia. This may include featuring a pale appearance and experiencing a weak feeling, as well as sudden hunger, a fast heartbeat, and convulsions. Some people tend to become confused and experience blurred vision whenever their blood glucose levels drop too low.
In more serious cases, a person may also lose their consciousness or even fall into a coma.
How These Conditions Are Linked
Now that we have provided a basic overview of both Hypothyroidism and Hypoglycemia, it is time that we take a look at how these two conditions may be linked.
Let’s start by looking at how an underactive Thyroid can cause a patient to experience Hypoglycemia. To understand this link, we need to look at what Hypothyroidism does to the body. In particular, we need to consider the effects of inadequate Thyroid hormone levels in the blood on glucose and insulin regulation.
When the Thyroid gland fails to secrete enough hormones to support vital functions in the body, then a patient may experience a reduction in the rate at which cells in their body take up glucose. The ability of the body to absorb glucose within the gastrointestinal tract also becomes impaired. Additionally, insulin response to high blood glucose levels become impaired as well, and it takes longer for the body to clear insulin from the patient’s blood circulatory system.
These effects cause cells to become deprived of adequate glucose levels; thus causing the Adrenal glands to secrete cortisol into the body. Cortisol is a hormone that is secreted in response to stress – low blood glucose levels is considered a stressful event by the body. When this happens, the functionality of the Thyroid gland is further suppressed as cortisol hormones are known to hurt the Thyroid’s ability to secrete an adequate level of hormones into the bloodstream.
This also explains how Hypoglycemia may lead to the development of Hypothyroidism, or cause Hypothyroidism to become worse in a patient that has already been diagnosed with the condition. When a patient experiences a low level of glucose in their bloodstream, and it is not caused by low Thyroid hormones, the Thyroid gland will still be affected by the cortisol hormones that are released by the patient’s Adrenal glands.
Additionally, it should be noted that individuals who frequently experience episodes of Hypoglycemia may also find that their Pituitary gland becomes impaired. The cortisol hormones cause an adverse reaction in the entire endocrine system – this includes the Pituitary gland. The Pituitary gland sits at the bottom of the brain and releases a number of different hormones – including Thyroid Stimulating Hormone.
Thyroid Stimulating Hormone, as the name of the hormone suggests, is responsible for stimulating the Thyroid gland. In turn, this tells the Thyroid gland to produce and release Thyroid hormones. When TSH is low, the Thyroid gland does not produce enough hormones to support overall cellular function.
This, in turn, causes the patient to experience symptoms of Hypothyroidism, due to the low levels of T4 and T3 in their blood.
The Most Appropriate Treatment Solution For These Conditions
When a patient is diagnosed with Hypothyroidism, and they experience Hypoglycemia, then the treatment of their condition becomes more complicated. Only treating one condition can make the treatment protocol less effective, as the other condition may still have an adverse effect on the particular condition that is being treated.
For this reason, a patient with Hypothyroidism is advised to become educated about the particular symptoms that may signal the presence of Hypoglycemia as well.
Screening for blood glucose levels and performing additional blood tests can assist with providing details regarding whether or not the low levels of Thyroid hormones in the patient’s body have affected the ability to regulate glucose and insulin effectively.
The purpose of the treatment protocol administered to a patient with both conditions is to help alleviate levels of Thyroid hormones in their body, while also assisting them with regulating and normalizing their blood glucose levels. This can be challenging, however.
When a treatment plan is provided that focuses on avoiding Hypoglycemia and to assist with providing an increase in Thyroid hormones, then adverse reactions may be observed in the patient’s blood glucose levels. When the Thyroid hormones start to become elevated in their body, their body’s ability to respond to insulin and the absorption of glucose within the patient’s cells may also become more effective. This may already make glucose levels more stable in the patient’s body but does not always. Should this be the case, then the addition of glucose stabilizing medication or techniques may then lead to elevated blood glucose levels in the patient.
In turn, this then places the patient at risk of Hyperglycemia. Hyperglycemia has been associated with many possible complications in the human body, including abdominal obesity, high blood pressure, chronic inflammation, and high cholesterol levels.
Insulin resistance is also more prevalent amongst individuals with Hyperglycemia than amongst individuals with normal blood glucose levels. Additionally, a patient with Hyperglycemia is also at a higher risk of blood clots.
The most effective method for providing an effective approach to treating these conditions together would be to target both through a single treatment plan and to provide close monitoring to the patient. Levels of TSH and T4, as well as blood glucose, should frequently be tested.
This can assist a physician in determining if the treatment plan is affected and also implement adjustments when they notice any adverse reactions caused by the treatment plan. If the treatments administered does not seem to be effective, dosage can be increased to better target the condition that does not seem to be affected by the medication provided.
Conclusion
Patients diagnosed with Hypothyroidism may be at a higher risk of developing Hypoglycemia. The connection between these two diseases is complex as, at the same time, a patient with Hypoglycemia may also be at risk of developing Hypothyroidism.
A better understanding of how these conditions can raise the chances of developing the other can help a patient better identify their risks. Furthermore, when additional symptoms are present that are not directly related to the diagnosed condition, a further understanding of this link can help a patient identify the possibility of the other disease being present.
This guide provided a comprehensive overview of the connection that is shared amongst Hypoglycemia and Hypothyroidism.
We looked at the symptoms of these conditions, as well as discussed how the conditions affect different functions in the body that may cause complications.
The presence of these two conditions at the same time need to be targeted carefully, as treating one condition without focusing on the other simultaneously may yield ineffective results.
References
1 M.P.J. Vanderpump. The epidemiology of thyroid disease. Oxford Academic: British Medical Bulletin. 1 September 2011. https://academic.oup.com/bmb/article/99/1/39/298307
2 Hypothyroidism (underactive thyroid). Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/hypothyroidism/diagnosis-treatment/drc-20350289
3 Hypothyroidism (Underactive). American Thyroid Association. https://www.thyroid.org/hypothyroidism/
4 Diabetes and Hypoglycemia. Diabetes CO UK. https://www.diabetes.co.uk/Diabetes-and-Hypoglycaemia.html

Warmest thanks
my strange unpleasant worrying symptoms are made unbelievably clear to me going for blood tests tomorrow .